Inflammation + Insomnia = Depression
An interesting study in older adults
An intriguing new study in JAMA Psychiatry looks at the role of inflammatory cytokines in mood changes and depression in older adults.
Some background, first:
Elevated inflammatory cytokines can be a root cause of depression, but only in some people. About 30% of older adults experience depression, and roughly half of them are prescribed antidepressant drugs, with SSRIs being the most common. One problem is that older adults are more likely to have adverse effects from antidepressants, ranging from increased falls to medication interactions. Additionally, most antidepressants are only slightly more effective than placebos on average.[ref][ref][ref]
Back to the new study:
The study participants were 160 adults over age 60 who didn’t have depression. However, some of the participants had long-term problems with insomnia. They were randomized to receive either IV saline as a placebo or a shot of endotoxin. (I’m not sure that I would have signed up for a clinical trial with an endotoxin injection!)
Endotoxin is a toxic lipopolysaccharide that is found on the outer membrane of certain bacteria. It triggers a strong inflammatory response in almost everyone.
The researchers then sampled the participants’ vital signs, did mood tests, and collected blood every hour for 9 hours. They also followed up over the next seven days with symptom questionnaires about mood changes.
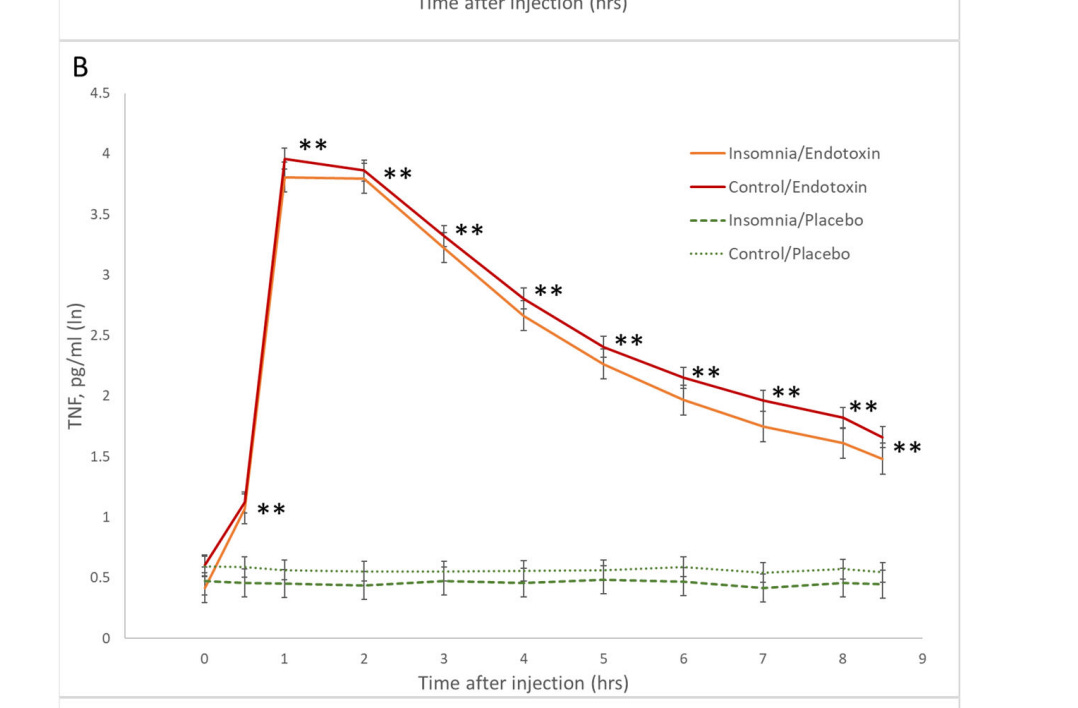
Administering endotoxin to older adults (or anyone) will almost always increase inflammatory cytokines, such as TNF and IL6. Here’s the dramatic increase in TNF-alpha within an hour of the endotoxin administration.
As you can see, the endotoxin injection did an excellent job of spiking inflammatory cytokines.
The researchers then followed up over the next hours and days to see if there were changes in mood and an increase in depressive symptoms. The study participants were divided up by whether or not they also had insomnia.
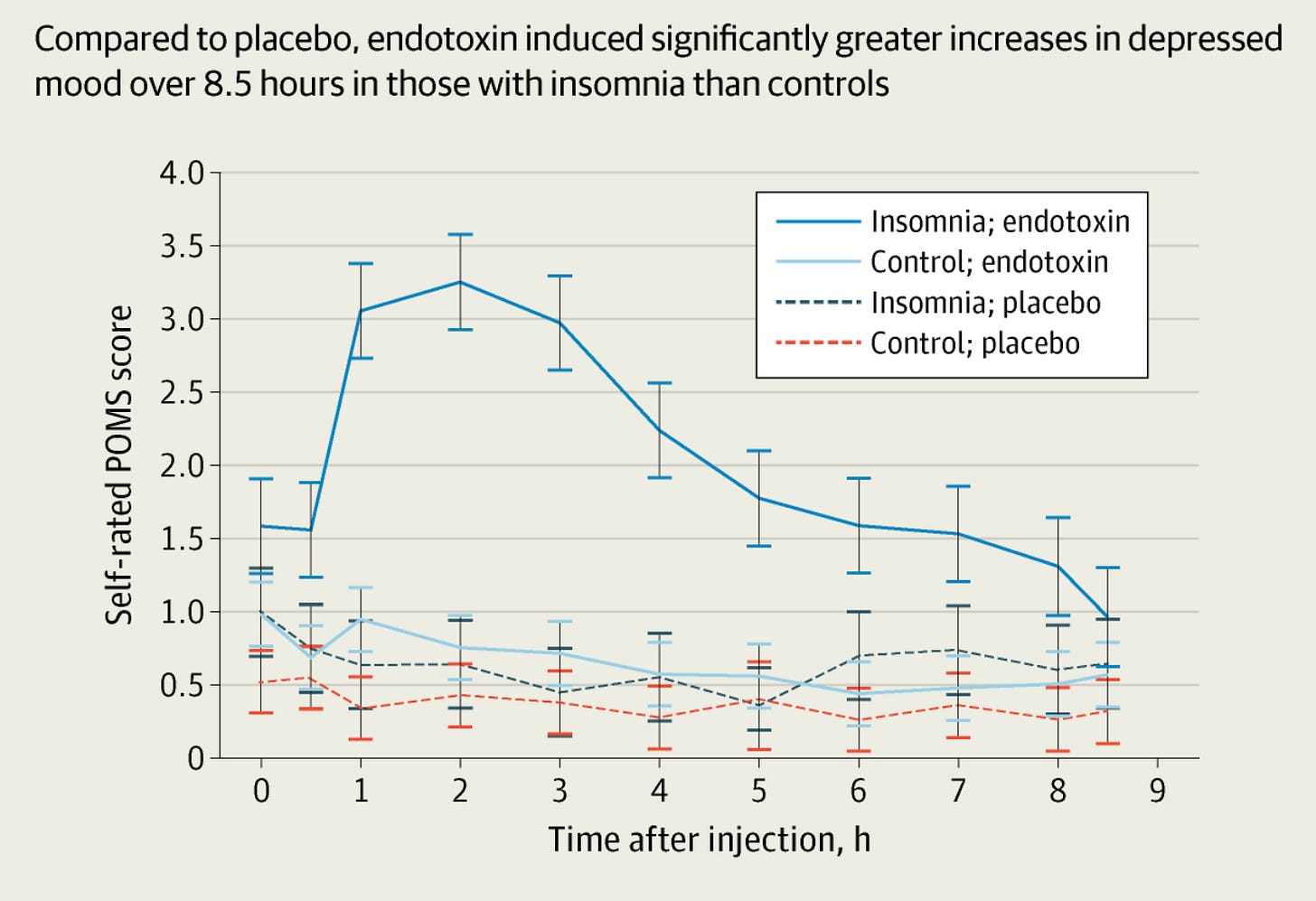
A clear pattern emerged showing that people with chronic insomnia were much more likely to have depression symptoms when their inflammatory cytokine levels rose. Conversely, individuals who hadn’t been dealing with insomnia did not have depression symptoms from the increase in inflammatory cytokines.
Why is this so interesting?
There are a lot of studies showing that inflammation causes some people to have depression - but not all. There are also studies showing connections between insomnia and depression. [ref][ref][ref]
This makes the connection between two hits - inflammation + insomnia - a clear risk for depression. Prior studies in younger adults also show that there is a two-hit link, but the researchers weren’t able to show causality.[ref]
How does this affect longevity and healthspan?
Sleep is important for overall health and wellness. This is something that we all instinctively know, but it is also good to quantify. Here’s what studies show:
A large study involving Americans over age 50 showed that for men, persistently higher insomnia scores increased the relative risk of all-cause mortality by over 70%. For women, the increased risk of death was only seen in those aged 50 -60 with higher insomnia scores.[ref]
Another study showed that in adults over 65, higher insomnia symptom scores were associated with a 26% increased risk of all-cause mortality.
Similarly, depression and mood disorders are a serious concern at any age, and especially in older age.
Mild to moderate depression also increases the risk of all-cause mortality, although there are a lot of confounding variables there.[ref]
Applications:
My takeaway from this is that if you are dealing with depression, consider whether you likely have elevated inflammatory cytokines and if you aren’t sleeping well.
Two options then emerge:
Sleep better
Tamp down inflammation
1) Curing insomnia: Sleeping through the night
There are multiple underlying causes of insomnia and no one-size-fits-all cures. Here are a few things, though, to look at and optimize:
Optimizing sleep environment: Sleeping in a cool, quiet room is important for quality sleep. If you live in a city or town, consider whether white noise, such as from a fan, would be helpful in maintaining sleep. Block out all light in your room while you sleep — blackout curtains, cover up the glowing indicator lights, wear a sleep mask (organic, silk) if needed, and if you have a clock, make sure it is red.
Put your mind to rest: An online clinical trial found that reading before bed improved sleep for 42% of people compared to 28% in the control group.[ref] Reading, especially a book that is only kind of interesting, helps to shift the mind into a relaxed state.
Block out blue light, increase melatonin: Light in the blue wavelengths stops the production of melatonin. Turning down overhead lights, switching lamps to an orange-tinted bulb, and shutting off electronics an hour or two before bedtime will do a lot for melatonin production and sleep quality. A low-dose, time-release melatonin supplement* may also help with maintaining sleep. (*Amazon affiliate links are just as an example. Read reviews and choose what’s best for you.)
Avoiding foods high in histamine: If you have a problem with maintaining sleep or with waking up too early, consider whether histamine intolerance and high-histamine foods could be playing a role. Histamine acts as a neurotransmitter in the brain and is involved in alertness. Excess histamine or levels of histamine rising too early in the morning can cause early-waking insomnia. (Genetic Lifehack’s article on Histamine Intolerance.)
Sleep aids: To some extent, waking up in the middle of the night or not being able to fall asleep can become a bad habit. It may be that some kind of sleep drug would help. However, the benzodiazepine-based sleep aids are not a good road to go down, since they are hard to quit. Zolpidem (generic Ambien) has also been shown to increase the relative risk of dementia and reduce glymphatic clearance.[ref][ref]
Over-the-counter options based on L-theanine, lemon balm, and melatonin may help. Benadryl for a short term (think weeks, not years) may also help you to retrain your brain to stay asleep. If you’re low in magnesium, a magnesium supplement may help.
This is not intended to be medical advice. Instead, I want to encourage you to keep trying multiple pathways, multiple options, if you have trouble sleeping. Everyone is different and something that works for a friend may not be the solution for you. Please talk with your doctor if you need medical advice.
2) Tamping down inflammation:
Again, a huge topic with no a one-size-fits-all answer.
Here are some starting points to consider:
Fish oil, krill oil, or Specialized Pro-Resolving Mediators: The resolution of inflammation is an active process that relies on lipid mediators derived from DHA and EPA. If you aren’t regularly eating oily fish, consider a DHA/EPA supplement. Read my whole article on specialized pro-resolving mediators.
Clean up your diet: While there are lots of different diets and an internet health guru claiming each is the best, the reality is that cutting out junk food and eating mainly whole foods is going to do a lot for reducing inflammation due to foods. You know what makes you feel sluggish after you eat it — clean that up.
Targeting TNF-alpha:
Decreasing IL1B:
Keeping IL-6 in check:
My point here is that there are quite a few natural ways to tamp down excessive inflammatory cytokines. You may need to try multiple ways or to reach out to a healthcare provider for help.
Conclusion
The new study on inflammation + insomnia causing depression symptoms is straightforward in showing that the combination is a bad one for most people.
To me, this is one of those nuggets of information to keep in the back of my mind. If/When I end up experiencing inflammation and insomnia, I’ll know that depressive symptoms are likely the result, and that addressing inflammation or sleep could resolve the triad of symptoms. This is something all of us are likely to experience at some point in life, so having a resolution plan should be helpful.